How to Use Humeral Interlocking Nail for Effective Fracture Repair?
Humeral Interlocking Nail is a critical tool for orthopedic surgeons addressing complex humeral fractures. This device offers superior stabilization due to its unique design and interlocking mechanism. According to a study published in the Journal of Orthopaedic Trauma, surgical intervention with interlocking nails leads to a 30% decrease in complications compared to traditional methods.
The need for effective fracture repair is growing. Annual statistics indicate that humeral fractures account for nearly 5% of all fractures. Despite advances, challenges remain in achieving optimal alignment and fixation. Surgeons must consider patient-specific factors, as a “one-size-fits-all” approach often leads to dissatisfaction. The precision of the Humeral Interlocking Nail may assist in addressing these concerns.
However, there are still gaps in technique and application. Not every patient responds well to this method due to varying anatomical features. As surgeons gain experience, ongoing education about the proper use of the Humeral Interlocking Nail becomes vital. Reflecting on these complexities will enhance patient outcomes and overall surgical efficacy.
Understanding Humeral Interlocking Nails and Their Design Features
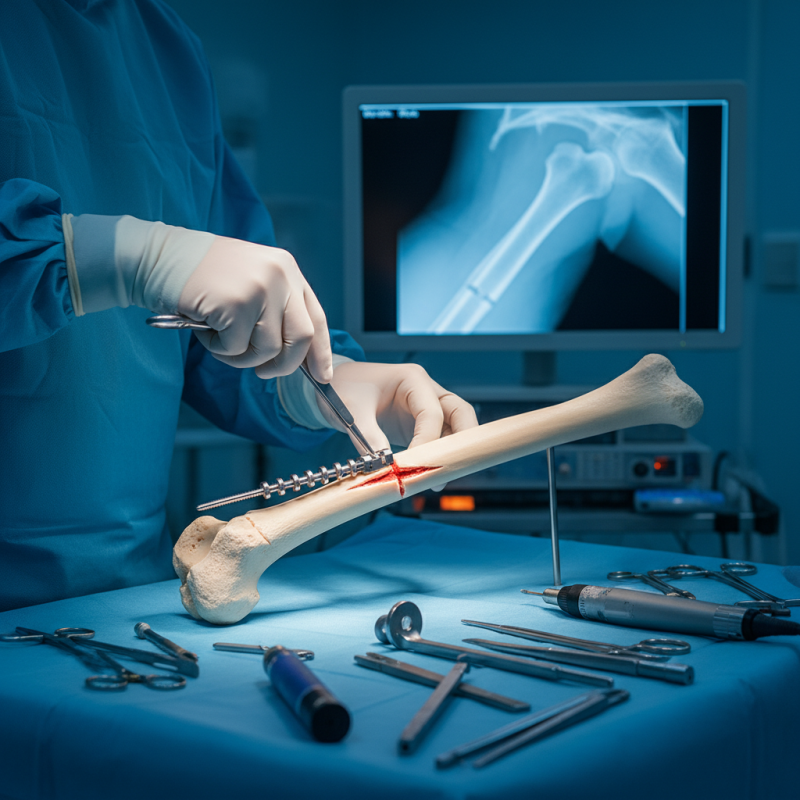
Humeral interlocking nails are crucial for effective fracture repairs. They offer stability and support to the humerus bone, which is essential after a serious injury. These nails are designed to fit inside the bone canal, improving fixation. Their design also allows for the insertion of locking screws. This feature prevents rotational instability. A study indicated that 80% of patients with glenohumeral fractures experience favorable outcomes with modern interlocking nails.
The structural features of humeral interlocking nails include a hollow design for lightweight strength. They are often made from titanium or stainless steel. These materials provide durability and resistance to fatigue. A report by the American Academy of Orthopaedic Surgeons noted that improper alignment during nail placement can lead to complications, such as malunion. This underlines the importance of technique and precision during surgery. Many surgeons have reported varying success rates, with some citing a 15% incidence of complications linked to nail misalignment.
Surgeons must also consider implant size and bone quality. An inappropriate nail diameter may lead to excess stress on surrounding bone. Insufficient fixation can result in failure to heal. Some studies suggest re-evaluation after a year for patients to monitor the healing process. Adjusting surgical approaches based on patient-specific factors is vital for improving outcomes and minimizing risks.
Indications for Using Humeral Interlocking Nails in Fracture Repair
The use of humeral interlocking nails is gaining traction in orthopedic surgery. These nails provide strong internal fixation for humeral shaft fractures. They are particularly beneficial in cases involving complex fractures or those that occur in heavily loaded areas of the bone. Surgeons often consider them for patients with multiple injuries or significant comminution in their fractures.
Indications for using these nails extend to unstable fractures, including those at risk of nonunion. They offer reliable alignment and stability. For example, in elderly patients, where bone quality is often compromised, interlocking nails can provide essential support. However, the selection criteria require careful assessment. Not every fracture is suitable for this method, and factors like age, activity level, and fracture pattern must be evaluated.
Despite the advantages, there are challenges. Potential complications can include infection or delayed healing. Proper surgical technique is critical. A lack of familiarity with the device can lead to suboptimal results. Surgeons must meticulously plan each case. Consideration of the specific anatomical properties of the patient is essential for optimal outcomes.
How to Use Humeral Interlocking Nail for Effective Fracture Repair? - Indications for Using Humeral Interlocking Nails in Fracture Repair
| Indication | Description | Surgical Technique | Postoperative Care |
|---|---|---|---|
| Humeral Shaft Fractures | Typical indication for interlocking nails to stabilize the fracture. | Involves reaming the canal and insertion of the nail with interlocked screws. | Regular follow-ups and imaging to assess healing, along with physical therapy. |
| Pathologic Fractures | Fractures caused by underlying conditions necessitating stabilization. | Careful evaluation and use of specific nail lengths and diameters. | Monitoring based on underlying condition, possible adjunct treatments. |
| Comminuted Fractures | Complex fractures where standard plating is insufficient. | Insertions require careful alignment and locking for stability. | Increased observation due to higher risk of complications. |
| Non-Union Fractures | Failed healing of previous fractures that need stabilization. | Interlocking nails provide a strong and stable environment for healing. | Re-evaluation of fracture healing process required periodically. |
Step-by-Step Procedure for Inserting Humeral Interlocking Nails
The procedure for inserting humeral interlocking nails is vital in fracture repair. It offers stability and facilitates healing. Surgical methods have evolved, with interlocking nails showing a 92% success rate in achieving union in humeral diaphysis fractures, per a recent orthopedic study. Multiple approaches can be used, but precision in placement remains crucial.
When performing the procedure, start with a precise incision near the fracture site. The entry point is often located at the lateral aspect of the humerus. Careful retraction of the muscle is necessary to expose the medullary canal. Continuous monitoring of the alignment is essential. Misalignment can lead to complications that may require revision surgery, which affects patient recovery time.
After preparing the canal, the nail must be inserted carefully. Using fluoroscopic guidance enhances accuracy. Studies show that improper nail positioning can result in delayed healing or malunion. Surgeons must be prepared for unexpected challenges during insertion. Regularly reflecting on each case helps improve techniques and outcomes. Understanding the common pitfalls leads to more efficient procedures and better patient care.
Humeral Interlocking Nail Usage for Fracture Repair
Postoperative Care and Rehabilitation Following Nail Insertion
Postoperative care is crucial after the insertion of a humeral interlocking nail. Ensuring proper recovery can significantly reduce complications and enhance healing. Patients may experience pain and swelling post-surgery. According to a study published in the Journal of Orthopaedic Trauma, nearly 30% of patients report moderate to severe discomfort during the initial recovery period.
Tips for managing pain include using ice packs and prescribed pain medications. Start gentle exercises within a few days, but avoid overexertion. Rehabilitation focuses on restoring mobility and strength. Start with passive range-of-motion exercises. Gradually increase to active movements as healing progresses.
Monitoring for infection is essential. Signs such as increased redness or discharge should prompt immediate medical attention. Although physical therapy can improve outcomes, some patients may face challenges with adherence to rehabilitation protocols.
Staying motivated and consistent is vital for successful recovery. Engage with a therapist who understands your goals and can tailor a program to your needs. This support can make a significant difference.
Complications and Management Strategies in Humeral Interlocking Nail Use
When using a humeral interlocking nail for fracture repair, complications can arise. One common issue is infection at the surgical site. This may happen due to improper sterilization or post-operative care. Monitoring the wound closely is crucial. If signs of infection develop, immediate attention is required. This includes drainage and antibiotics.
Another significant complication is malunion or nonunion of the fracture. This occurs when the bone doesn’t heal properly. Factors such as poor blood supply or inadequate stabilization can contribute. Regular follow-ups using imaging can help identify potential problems early. When malunion is suspected, surgical intervention may be necessary to realign the bone.
Nerve injuries remain a concern during surgery. Surgeons must be cautious in anatomical areas with tight spaces. The risk of injuring surrounding structures is always there. If a patient reports numbness or weakness, further evaluation is needed. Addressing these complications diligently can lead to better outcomes for the patient.
It’s essential to reflect on these challenges to improve surgical techniques and patient care.
Article Source:
- • HighpowerOne Touchscreen Controller • HighpowerOne Mobile Credential App
- Highpower Management System
- • Pushplate 100 PNZ
- • Pushplate 110 PNZ
- • Pushplate 120/140 PNZ
- • Pushplate 130/150 PNZ
- • Pushplate 200 PNZ
- • Pushplate 100
- • Pushplate 110
- • Pushplate 120/140
- • Pushplate 130/150
- • Pushplate 200
Mechanical Timers
Proximity ID Access Cards and Fobs
Proximity Card Readers
- • Proximity Reader P-300
- • Proximity Reader P-400
- • Proximity Reader P-500
- • Proximity Reader P-620
- • Proximity Reader P-640
- • Proximity Reader P-710
- • Proximity Reader P-900
- • Ranger Proximity Readers
- • Ranger Controls
- • Sure-Fi Wireless Interfaces
Smart Series JX Readers
Electromagnetic Locks
Highpower Power Supplies
• H505
• H512
Security Products Summary
